Nursing Iraq back to health

MAZIN Al Mazini is still haunted by the memory of the teenager he tried to save.
He had been working at Baghdad Teaching Hospital for just three months when a young man was brought in having lost both his legs in a bomb attack in the city centre.
Advertisement
Hide AdAdvertisement
Hide Ad“I can’t forget that boy,” says the 28- year-old anaesthetist technician. “He was about 17 years old and came from a rich family and I believe he had a lot of dreams for the future.”
The teenager had just parked his car and popped into a shop when the bomb exploded, ripping him and his car apart. “When I received him he was really pale and lost a lot of blood. Even when we anaesthetised him he was still shivering from the pain, it was really terrible,” adds Mazin.
“I spent as long as 18 hours a day just on that boy to try and save his life, especially when I saw his mum and sister.” Mazin and his medical colleagues managed to keep him alive for three weeks before he finally succumbed to his injuries.
This was back in 2006, at the height of the sectarian violence in Iraq when suicide bomb attacks were an almost daily occurrence. The situation has improved since then, although according to the United Nations at least 7,818 civilians were still killed in violent attacks across the country last year.
Advertisement
Hide AdAdvertisement
Hide AdThe violence has put the nation’s struggling healthcare system under immense pressure and as a result the Iraq Ministry of Health has sent some of its brightest medical staff, like Mazin, abroad to learn new skills which it is hoped can help improve medical care in Iraq.
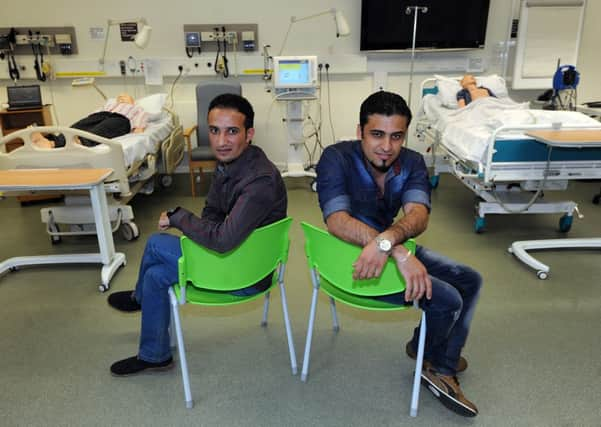
The UK is among those involved and for the past two years Sheffield Hallam University has been running a project, funded by the Iraqi government, which has seen 138 Iraqi nurses, doctors and physicists learn about the NHS and gain hands-on experience in the city’s hospitals.
Mazin was among the first group of Iraqis that came to South Yorkshire in 2012. In their initial visit the medical staff spent most of their study time improving their English, but on their return visits they have concentrated solely on developing their medical expertise and learning how the healthcare system works in this country.
Mazin says he has learned a great deal during his time in England, not just practical medical techniques but also teamwork and communication skills. “It’s important to communicate with the patients as well as with doctors and colleagues. The main goal of being here in the UK is to improve things back in Iraq and we have learned to share what we learn so at the end we all have a rich base of information and knowledge.”
Advertisement
Hide AdAdvertisement
Hide AdBut while he and his colleagues have been inspired by their time in Sheffield, there are still many challenges facing the healthcare system back in his homeland.
“There has been about 35 years of corruption in Iraq,” Mazin adds. “Over the years this has led to some of its most talented young professionals leaving the country in search of a better life. We had a lot of qualified nurses, technicians and doctors who left to go to the US, or the UK and Australia to find good jobs.”
This has undermined attempts to improve the medical profession in Iraq, but the hope is that programmes like the one in Sheffield will make a difference in the years to come.
Mohammed al Duraye is a 25-year-old nurse from Baghdad who has returned to Sheffield for the second part of his course and is here until the end of June. He, too, is full of admiration for the NHS.
Advertisement
Hide AdAdvertisement
Hide Ad“In the UK the nursing is very organised, nothing is done randomly. This is different from my country so we have to learn how to organise our work better,” he says.
While in Sheffield the students have been on observational visits to hospitals as well as being given the opportunity to put their skills to practice. “Teaching at the university is very good and you are made to feel like an equal,” Mohammed says.
“We’ve seen all kinds of nursing, we’ve seen specialists, consultants and registrars but in our country we only have a general nurse, we don’t have these specialities. But this is something we want to transfer back to Iraq.”
Mohammed, one of seven brothers and sisters, says that in Iraq a lot of people study to become a nurse because it gives them a guaranteed job, rather than doing it because it’s something they’re passionate about.
Advertisement
Hide AdAdvertisement
Hide Ad“Many of them don’t like their work and that is something we need to change. We need to encourage our colleagues to love their job because to give good care to people you have to enjoy what you do.”
In Iraq you either train to become a nurse or a doctor but Mohammed would like to see such rigid divisions done away with. “It’s important that people are encouraged to learn more and to develop their skills and that is why I try to learn as much as possible so that I can give the best care I can.”
But he admits this isn’t easy with the security issues and the threat from insurgents and suicide bombers which continues to make life fraught for medical staff in Iraq.
“It’s a difficult situation but nurses work hard every day,” he says. “The Ministry of Health is doing its best to improve things. As a nurse I have seen an improvement from year to year so if we compare the situation from 10 years ago it’s much better now.”
Advertisement
Hide AdAdvertisement
Hide AdMazin, too, sees some cause for optimism on the back of what he has learned from his time in Sheffield. “When somebody loses a bit of their body it’s so easy for it to get infected and when I came to Sheffield I heard about something called infection control. Here they have a huge number of people working on this but back in Iraq we don’t have that.”
However, this is something he is already looking to change. “In the gap between the two courses I talked to the manager, who was a surgeon, and told him about what we had learned, including infection control and that we could employ some people to work on this.”
On top of this he has started running regular lectures for his colleagues, talking about some of the different skills and approaches used in the UK and how they might help them.
It’s these kind of improvements that gives him and his colleagues hope for the future. “There has been many years of corruption to the foundations of Iraq, especially to the medical and healthcare institutions. But after another 10 or 15 years I think we will have made good steps forward,” he says.
Advertisement
Hide AdAdvertisement
Hide Ad“I’m optimistic for the future. If we can send more people here to get new qualifications and a new vision for the future of nursing it can make a difference. This is important because the Iraqi people deserve something more than what they have.”
That way if somebody is brought to him with terrible injuries in the future, next time he might be able to help save them.