Andrea Jenkyns: Malaria-free world will boost economies


I recently travelled to Kenya with Malaria No More UK to gain a deeper understanding of the impact of malaria and how we can beat it. Sadly, the human cost of the disease was most evident on Siaya County Hospital’s children’s ward. Doctors and nurses were treating several young children that were unconscious with severe malaria.
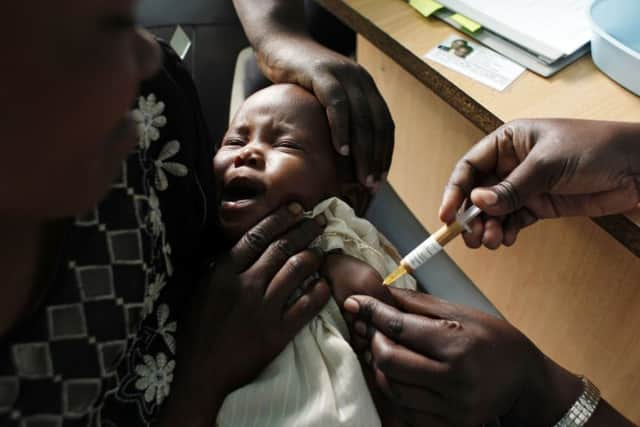
Statistics show that a child dies every two minutes from Malaria, and it was heartbreaking to see that, often, by the time families travel to their nearest health facility, it can be too late. As a mother myself to a young toddler, to witness a baby needing to be resuscitated due to this terrible disease brought tears to my eyes.

Advertisement
Hide AdAdvertisement
Hide AdHowever, in Siaya County, volunteers have been trained to diagnose and treat malaria in their own communities, thus thankfully preventing complications and deaths.
I saw first-hand how this approach is saving lives. On a home visit, I saw how simple it is to test and treat malaria if the right medicines are made available. It took 20 minutes to test three-year-old Rollins, and within the hour Rollins had been treated and was on the road to recovery.
Despite malaria being treatable and preventable, it still claims 500,000 lives every year and is the world’s oldest and deadliest disease. There has been a significant reduction in cases and deaths, but now, for the first time in a decade, progress has stalled and there is a risk of resurgence.
One of the biggest threats to progress is the development of antimicrobial resistance, which my own father died from following a routine operation. Resistance to artemisinin drugs, the most powerful drugs currently available to treat malaria, has now been found in five countries in South-East Asia.
Advertisement
Hide AdAdvertisement
Hide AdBritain has been at the forefront of the malaria fight through political leadership, funding and science and research, like the new insecticides at Liverpool’s Innovative Vector Control Consortium and GSK’s development of the world’s first vaccine against malaria.
With this experience and resource, the UK is in a unique position to demonstrate leadership on the fight against malaria. The UK has strong economic, political and cultural links with many of the countries most affected by malaria, not least through membership of the Commonwealth.
Ninety per cent of Commonwealth citizens live in malaria endemic countries. We cannot end this killer disease without Commonwealth action. In April Commonwealth countries signed up to halving malaria by 2023. If realised, the impact would be immense: 350 million cases would be prevented, and 650,000 people saved. The UK Government holds the privileged position of Commonwealth Chair-in-Office for the next two years and must use this opportunity to work with Commonwealth members to maximise progress.
UK leadership tackling malaria epitomises global Britain at its best, a nation that is an outward looking force for good in the world, leading the way in tackling the great challenges facing the world’s poorest people. It is also in our national interest. An EY report estimates that UK trade with the 13 most malaria-affected countries could have been up to £765 million higher in 2015 but for the effects of malaria.
Advertisement
Hide AdAdvertisement
Hide AdAs the UK strengthens ties with the Commonwealth and seizes opportunities to forge a new set of trade and investment relationships post Brexit, driving progress towards a malaria-free world will address a significant barrier to economic development and, ultimately, boost UK trade.
We must end this deadly disease once and for all.
Andrea Jenkyns is the Tory MP for Morley and Outwood.