Tim Farron: It is our duty to make cancer care accessible to all, including rural areas
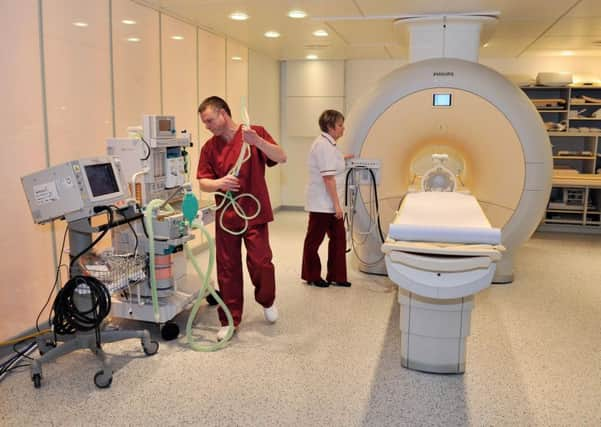

I start by paying tribute and saying a massive thank you to those NHS professionals who work tirelessly up and down the country, day in and day out, to look after us and our loved ones when we need it most. I especially want to put on record my appreciation for those who work in cancer care.
We have some of the best cancer care in the world, but here is the problem. Yes, we have world-leading treatment, but it is not truly available equally. The availability of care depends hugely on people’s ability to access it.
Advertisement
Hide AdAdvertisement
Hide AdI welcome the £130m announced by NHS England that is to be invested in improving radiotherapy treatment. Working in clinical networks and developing specialised services has a strong evidence base, but what is not addressed is the inequality in access to services that already exist.
That inequality will only get worse if it is not addressed now by NHS England. I am grateful to the Government that the consultation into allocating that investment has been extended to January 24, not least because it gives the Minister the chance to amend the criteria and the priorities for allocating services.
I passionately believe that one of the criteria in allocating improved radiotherapy services must be the shortening of the distances that people have to travel, especially for those with more common cancers.
My position is backed up by evidence, including a publication in the British Medical Journal in 2016 indicating that outcomes are worse for people who need to travel further. Let me be clear what “worse outcomes” actually means. Worse outcomes can mean patients actively deciding to forego potentially life-saving or life-lengthening treatment because getting to hospital is just too much of a trauma for them owing to the length and difficulty of the journey that is required.
Advertisement
Hide AdAdvertisement
Hide AdWorse outcomes means choosing forms of treatment that may be less effective than radiotherapy because the nearest unit is too far away. Worse outcomes includes patients failing to complete a vital course of radiotherapy treatment because they simply cannot cope with the gruelling, wearying travelling every single day.
Action Radiotherapy estimates that one in six of us will need radiotherapy to treat cancer at some point in our lives, but easy access to this treatment can depend entirely on a postcode lottery. It is the sad reality that in rural areas of England travel times to cancer treatments can be unbearably long for too many people, and patients are often forced to cover these long distances on public transport.
Not everyone has the option of travelling in the relative comfort of a personal car, and even if a person does, driving themselves or being driven, day in and day out for four to six weeks, is a massive challenge. I believe that it is frankly cruel to force people who are already very poorly to make a two or three-hour round trip every day, for weeks, in order to receive life-saving care.
In its 2007 report, the National Radiotherapy Advisory Group recommended that cancer patients should have to travel no more than 45 minutes one way – an hour and a half both ways – to receive radiotherapy treatment. This was adopted in the service specification by NHS England, but has since disappeared. Experts in the field maintain that travelling any longer could have a hugely negative impact on treatment outcomes and patient wellbeing.
Advertisement
Hide AdAdvertisement
Hide AdIf preventing unacceptable travelling times became a part of NHS England’s criteria for delivering radiotherapy, it would hugely increase our chances of bringing a radiotherapy satellite unit to Westmorland General Hospital in Kendal in my constituency.
Radiotherapy treatment at Westmorland General Hospital is long overdue and would mean the world to local people, who now have to make the long journey to Preston for treatment. Let us be clear: the Rosemere unit in Preston is excellent – my own mother received wonderful treatment there – but for most people in south Cumbria, it is ludicrously distant.
For some people living in the remotest areas of my part of the world who are eligible for hospital-provided pick-ups, a round trip to access treatment in Preston, including waiting times, could easily surpass six hours.
Requiring NHS trusts to make it a priority for investment to ensure that radiotherapy is available more locally – such as by bringing a satellite unit to our local hospitals – would significantly improve outcomes for patients.
Advertisement
Hide AdAdvertisement
Hide AdMy request is simple. I want travel times and equality of access, particularly for people who are older or who have disabilities, to be key criteria when allocating cancer services.
Tim Farron is the former Lib Dem leader and MP for Westmorland and Lonsdale. He led a Parliamentary debate on Cancer Treatment: Patient Travel Times. This is an edited version.