How does the Covid vaccine work and why has it been approved so quickly? Your questions answered
It could be rolled out in Leeds as early as next week, with health and care workers, people over 80 and care home residents the first to get a vaccine.
The mass-vaccination of the public in Leeds is due to start early next year.
Advertisement
Hide AdAdvertisement
Hide AdBut how does it work and why has it been approved so quickly?


Here's everything you need to know:
– Is this a reason to celebrate?
Yes. Analysis shows the vaccine can prevent 95% of people from getting Covid-19, including 94% in older age groups.
The vaccine has been tested on 43,500 people in six countries and no safety concerns were raised.

Approval means the UK can begin rolling out the vaccine to those most in need, including frontline NHS workers.
– What type of vaccine is this?
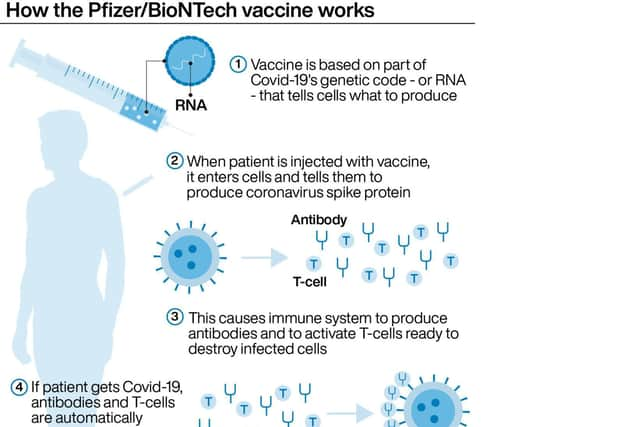
The jab is known as a messenger RNA (mRNA) vaccine.
Advertisement
Hide AdAdvertisement
Hide AdConventional vaccines are produced using weakened forms of the virus, but mRNAs use only the virus’s genetic code.
An mRNA vaccine is injected into the body where it enters cells and tells them to create antigens.
These antigens are recognised by the immune system and prepare it to fight coronavirus.
– What are the advantages of this type of vaccine?
No actual virus is needed to create an mRNA vaccine. This means the rate at which it can be produced is dramatically accelerated.
Advertisement
Hide AdAdvertisement
Hide AdAs a result, mRNA vaccines have been hailed as potentially offering a rapid solution to new outbreaks of infectious diseases.
In theory, they can also be modified reasonably quickly if, for example, a virus develops mutations and begins to change.
mRNA vaccines are also cheaper to produce than traditional vaccines, although both will play an important role in tackling Covid-19.
One downside to mRNA vaccines is that they need to be stored at ultra-cold temperatures and cannot be transported easily.
– Are they safe?
Advertisement
Hide AdAdvertisement
Hide AdAll vaccines undergo rigorous testing and have oversight from experienced regulators.
Some believe mRNA vaccines are safer for the patient as they do not rely on any element of the virus being injected into the body.
mRNA vaccines have been tried and tested in the lab and on animals before moving to human studies.
The human trials of mRNA vaccines – involving tens of thousands of people worldwide – have been going on since early 2020 to show whether they are safe and effective.
Advertisement
Hide AdAdvertisement
Hide AdPfizer will continue to collect safety and long-term outcomes data from participants for two years.
– Do we have enough doses to vaccinate the UK population?
The UK has secured 40 million doses of the Pfizer/BioNTech vaccine, with 10 million due in the UK by the end of the year.
Patients need two doses, meaning not enough shots have been secured for the entire UK population.
However, it is likely other vaccines, including one from Oxford University, will be approved in the coming weeks and months.
Advertisement
Hide AdAdvertisement
Hide AdTraditionally vaccines can take years to research and develop, so how has a vaccine been approved for use so quickly?
– How has this come about so quickly?
The timetable for developing and approving a Covid vaccine has been condensed due to the coronavirus crisis.
– What is the usual process for developing a vaccine?
Traditionally vaccine development takes several years and includes various processes, including design and development stages followed by clinical trials – which in themselves need approval before they even begin.
The trials take place in three sequential stages – also known as phases. The research will show whether a vaccine generates antibodies but also protects people from disease. They will also identify any safety issues.
Advertisement
Hide AdAdvertisement
Hide AdOnce the trials are complete, the information gathered by researchers is sent to regulators for review.
This is thoroughly analysed by clinicians and scientists before being approved for widespread use.
Then, after approval from regulators, people can start to receive the vaccine.
– Is this different because of the pandemic?
The process looks slightly different in the trials for a Covid vaccine.
Advertisement
Hide AdAdvertisement
Hide AdWhile the early design and development stages look similar, the clinical trial phases have overlapped – instead of taking place sequentially.
– But won’t that mean that safety is compromised?
Even though some phases of the clinical trial process have run in parallel rather than one after another, the safety checks have still been the same as they would for any new medicine.
The Medicines and Healthcare products Regulatory Agency (MHRA) has adopted the phrase “safety is our watchword”.
Regulators have said they will “rigorously assess” the data and evidence submitted on the vaccine’s safety, quality and effectiveness.
Advertisement
Hide AdAdvertisement
Hide AdAnd, in most clinical trials, any safety issues are usually identified in the first two to three months – a period which has already lapsed for most vaccine frontrunners.
– How are regulators acting so quickly?
Regulators have been carrying out “rolling reviews”, which means that instead of going through reams of information at the conclusion of the trials, they have been given access to the data as the scientists work.
A rolling review of the vaccine data started several months ago.
This means regulators can start to look at scientific data earlier than they traditionally would do, which in turn means the approval process can be sped up.
Advertisement
Hide AdAdvertisement
Hide AdRegulators sometimes have thousands of pages of information to go over with a fine-tooth comb – which understandably takes time.
Once all the data available on the vaccine is submitted, MHRA experts will carefully and scientifically review the safety, quality and effectiveness data – how it protects people from Covid-19 and the level of protection it provides.
After this has been done, advice is sought from the Government’s independent advisory body, the Commission on Human Medicines (CHM).
– What does ‘approved for use’ mean?
For a medicine to be used in the UK it has to be granted a licence. This means that it has been through all the rigorous safety and efficacy checks and regulators are confident in the findings of the clinical trials.
Advertisement
Hide AdAdvertisement
Hide AdBy reviewing the data as they become available, the MHRA can reach its opinion sooner on whether or not the medicine or vaccine should be licensed without compromising the thoroughness of their review.
– So what data will the regulator look at?
The information provided to the MHRA will have included what the vaccine contains, how it works in the body, how well it works and its side-effects, and who it is meant to be used for.
This data must include the results of all animal studies and clinical trials in humans, manufacturing and quality controls, consistency in batch production, and testing of the final product specification.
The factories where the vaccines are made are also inspected before a licence can be granted to make sure that the product supplied will be of the same consistent high standard.
– What is the difference between the MHRA and the CHM?
Advertisement
Hide AdAdvertisement
Hide AdThe MHRA is the British regulator of medicines and medical devices, ensuring their safety, quality and effectiveness.
The CHM advises ministers on medicinal products. It is made up of an independent group of advisers responsible for advising on the need for, and content of, risk management plans for new medicines.
It also advises officials on the impact of new safety issues on the balance of risks and benefits of licensed medicines.
The CHM also offer advice on “applications for both national and European marketing authorisations”.
Advertisement
Hide AdAdvertisement
Hide Ad– Haven’t pharmaceutical companies already started making vaccines?
Yes. Usually large-scale production and distribution begins only after regulatory approval. But in the case of Covid-19 vaccines, pharmaceutical firms have begun manufacturing before final approval had been granted – taking on the risk that they may be forced to scrap their work.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.