GP surgeries failing to provide 'appropriate' level of in-person appointments to be named and shamed in new league tables
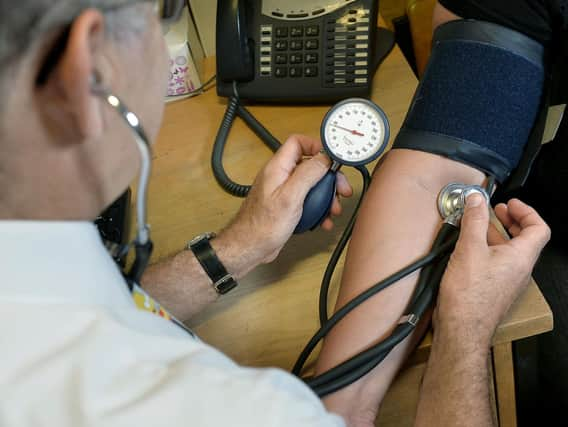

GP surgeries which fail to provide an appropriate level of “access” will be named and shamed in league tables as patients are given a new right to demand face-to-face appointments.
The NHS is ploughing millions of pounds into a new package of measures aimed at improving access to GPs, but practices which fail to provide an “appropriate” level of face-to-face appointments will not be eligible for the new funding.
Advertisement
Hide AdAdvertisement
Hide AdThe British Medical Association (BMA) condemned the plans, with General Practitioners Committee chairman Dr Richard Vautrey saying: “GPs across England will be truly horrified that this is being presented as a lifeline to general practice, when in reality it could sink the ship altogether.”
The Royal College of GPs (RCGP) called on the Government to fulfil its manifesto pledge of an additional 6,000 GPs and 26,000 other primary care professionals in the workforce by 2024 – a target that is highly likely to be missed.
Professor Martin Marshall, chair of the RCGP, said: “We know some patients prefer to see their GP face to face – but good care can and is being delivered remotely and some patients prefer it.”
Meanwhile, TV doctor and GP Rosemary Leonard accused Health Secretary Sajid Javid of “stirring up anti-GP rhetoric”, adding that there are not enough locums to employ to plug the gaps.
Advertisement
Hide AdAdvertisement
Hide AdUnder the new plans, patients will be able to rate their GP practice’s performance via text message.
The measures will also see GPs freed from some red tape, and other parts of the NHS will be called upon to help with some care – such as other healthcare workers being given new powers to provide patients with fit to work notes or DVLA checks.
NHS England said the measures, including a £250 million winter access fund, will enable GP practices to improve availability and increase the number of face-to-face appointments and same-day care.
The blueprint for improving access, published by NHS England working closely with the Department of Health and Social Care, includes a number of measures including:
Advertisement
Hide AdAdvertisement
Hide Ad– The new investment will fund locums as well as support for GPs from other health professionals such as physiotherapists and podiatrists.
– The NHS said GP practices must “respect preferences for face-to-face care unless there are good clinical reasons to the contrary”.
– Local health systems will be given some freedom to determine how to tackle access problems, which could include “walk-in consultations”.
– But the NHS will “increase its oversight” of practices with the most acute issues in relation to access, it said.
Advertisement
Hide AdAdvertisement
Hide Ad– GP appointment data will be published at practice level by spring – so people will be able to see how well their surgery performs compared to others. The NHS said this will “enhance transparency and accountability”.
– Practices which do not provide “appropriate levels” of face-to-face care will not be able to access the additional funding and will instead be offered support. Though it is not clear what the level of appointments need to be face-to-face.
– The money will help upgrade GP surgery telephone systems – which will hopefully drive down long waits on the phone.
– The Government will reform who can provide medical evidence and certificates such as fit notes and DVLA checks – freeing up more time for appointments.
Advertisement
Hide AdAdvertisement
Hide Ad– Infection control will be assessed which is likely to lead to social distancing in practices being changed or downgraded.
– Patients will also be able to see different types of clinicians in general practice including nurses, pharmacists and paramedics.
Amanda Pritchard, chief executive of the NHS in England, said: “Improving access to high quality general practice is essential for our patients and for the rest of the NHS too.
“It is a personal priority and today NHS England is taking both urgent and longer term action to back GPs and their teams with additional investment and support.”
Advertisement
Hide AdAdvertisement
Hide AdMr Javid said: “I am determined to ensure patients can see their GP in the way they want, no matter where they live.
“I also want to thank GPs and their teams for their enormous efforts in the most challenging times in living memory.
“Our new plan provides general practice teams with investment and targeted support.
“This will tackle underperformance, taking pressure off staff so they can spend more time with patients and increase the number of face-to-face appointments.
Advertisement
Hide AdAdvertisement
Hide Ad“Alongside this we are setting out more measures to tackle abuse and harassment so staff at GP surgeries who work so tirelessly to care for patients can do so without having to fear for their safety.”
It comes after campaign group EveryDoctor, which represents 1,700 UK doctors, said that GPs have been “blamed” for the proportion of telephone consultations offered to patients when they had been instructed by the Government to offer initial consultations on the phone or online.
Dr Julia Grace Patterson, chief executive of EveryDoctor, told a briefing on Wednesday: “It’s a bit of a shock for GPs to have been told vehemently by the Health Secretary last year that all appointments should be via telephone, and now we are told the absolute opposite and, in fact, blamed for the amount of telephone consultations that have been happening.”
In July last year, then Health Secretary Matt Hancock said that all initial GP appointments “should be teleconsultations unless there’s a compelling clinical reason not to”.
Advertisement
Hide AdAdvertisement
Hide AdAnd the NHS’s Long Term Plan, published in 2019, put forward proposals for all patients to be given a “digital-first” option for accessing GP care, should they want it.
Official figures show that 58% of GP appointments in England in August were face-to-face.
Before the pandemic, in August 2019, four in five appointments were carried out in person.
In September, leading GPs said that the current balance of face-to-face appointments was “about right”.
Advertisement
Hide AdAdvertisement
Hide AdBut a new YouGov poll suggests that two-thirds of people would prefer a face-to-face appointment.
When asked which type of GP appointment they would prefer, the survey of 5,400 British adults found that 66% would prefer a face-to-face appointment, 5% would like a video consultation and 25% said they would not mind what type of appointment they would receive.
EveryDoctor also expressed concern that “inflammatory” rhetoric about access to GP services was leading to “abuse” of staff.
The new blueprint will also include action on new efforts on how to tackle abuse of staff.
The NHS said it will work with the Academy of Medical Royal Colleges to develop a zero-tolerance campaign on abuse of NHS staff, including GP teams.