Nurse Pauline Cafferkey’s Ebola diary

Pauline Cafferkey is an associate public health nurse at Blantyre Health Centre in South Lanarkshire.
She has been a nurse for 16 years and says she was inspired to go into the profession after seeing images of the Ethiopian famine on the television in the 1980s. So she felt compelled to volunteer with Save the Children to help with the Ebola crisis, which has claimed the lives of more than 7,000 people to date. Pauline flew out to Freetown in Sierra Leone in November, along with another four Scottish volunteers, as part of a UK group of 30 NHS medical staff.
Advertisement
Hide AdAdvertisement
Hide AdHere is her moving first person diary piece recording her first four weeks on the front line in the battle against the deadly disease.
Week one: From the minute I step off the plane in Sierra Leone, the smell of chlorine hits me and a thermometer is pointed at my head. Fortunately this is by no means a bad thing. As part of the group of 30 NHS staff who left the UK we have gone our separate ways and I am with a group of 14 working with an NGO (non-government organisation/charity) just outside the capital, Freetown.
We are very well catered for and are housed in a wee shack on the beach. It has electricity for a few hours during the night and although mostly cold has running water. This is basic stuff but I’m not here for a holiday. Being coastal we are very fortunate to get to walk along a beautiful beach every day to get to the hotel that serves our food.
Although I don’t get to see a great deal of Sierra Leone, from the journey to work and the area surrounding where we are staying, I can tell it is a country of immense natural beauty. Not only that, but we pass a small mangrove with crocodiles every day, not your average walk to work. After nine days of training in the UK it feels good to eventually set foot in the Ebola Treatment Centre and begin work.
Advertisement
Hide AdAdvertisement
Hide AdThe area where the Ebola patients are is classed as the infective Red Zone, and the area surrounding it, the safe Green Zone. Bizarrely we find ourselves saying “good luck” to our colleagues prior to entering the Red Zone, a sobering reminder of what we are doing.
I was ill the other day, either from over-hydration as not enough salts in my body or heat exhaustion. It’s very difficult to judge the amount of fluid needed as the quantities we loose are immense. The ORS [oral rehydration salts] which get added to water to help balance out the body’s salt and sugars that are being lost are not the most palatable. I vomited out of the minibus window on the way home – luckily I managed to avoid any splash back and being decapitated.
Week two: Feel like the work I am doing is a normal part of life. My nice community- nursing job in Blantyre is far removed from this but at the moment this seems a lot more real. The dreams that I do remember always seem to have an Ebola theme, it seems to be all consuming.
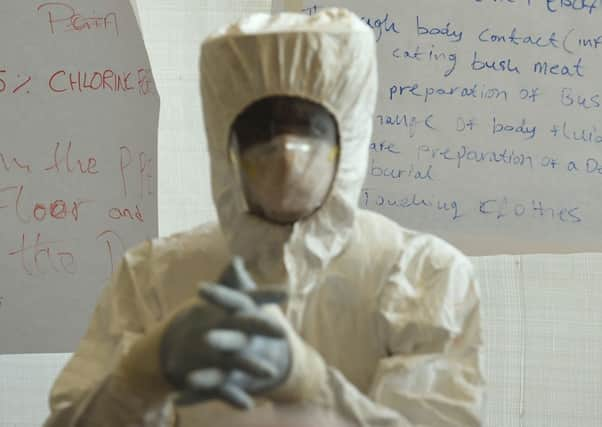
The PPE [personal protective equipment] alien-type suit that I have to wear when going into the positive Red Zone is horrendous. It takes about 20 minutes to dress and 15 minutes to take the suit off at the other end. They would certainly be beneficial on a cold winter’s night in Scotland but working in them in 30-degree heat is uncomfortable to say the least. On the up side, I feel very well protected. I was unaware that I could sweat so much. When I get to the decontamination area and remove the suit and gloves, there are pools of sweat dripping from me and not a dry hair on my head.
Advertisement
Hide AdAdvertisement
Hide AdI feel sorry for the poor patients who have these alien-type people caring for them. Especially so for the young children, who are not only very sick but have these strange creatures with only their eyes visible trying to make them drink and take medications.
Week three: Had an awful shift this week. I was with a lady who was dying. I could tell she didn’t have long, so I was trying to make her comfortable. There was a young boy standing at the window looking in and I waved to him. A few minutes later she had passed away and I heard the boy crying outside the ward. When I went to him, he asked if she had died. I said yes. He said she was his mother. He had already lost his father to Ebola, and now he had no parents. I tried to console him, and he said he has a sister who also came to the treatment centre with him and his mother, but he did not know where she was. A young girl had died that morning. I could not be one hundred per cent sure that it was his sister, so I wasn’t able to offer him any news. I took him back to his ward and gave him a drink.
On leaving the Red Zone I checked the notes and confirmed that the girl who died that morning was his sister. His mother had seen her daughter die in the bed across from her that morning and she died a few hours later. I informed the psychologist of the young boy and she will offer support. The sad thing is that this is a regular occurrence and we see and hear of whole families being wiped out by this awful disease.
Week Four: Not long till Christmas, there is no sign of anything Christmassy. Apparently the government have banned any Christmas and New Year gatherings. Apart from the obvious impact on health, Ebola is multifaceted in its destruction, with high unemployment and many orphans. The schools have been closed for some time now and it doesn’t look like that they will be opening any time soon.
Advertisement
Hide AdAdvertisement
Hide AdThe Sierra Leonean’s are normally very tactile people who, prior to Ebola would hug and shake hands as a normal greeting and now have to change their culture. Even for us NHS staff, when we accidentally touch each other we call out “no touch” in a humorous manner.
The already very busy treatment centre will be getting a lot busier in the next few days as the government have started doing house-to-house searches for those who are potentially infected. As there is still a lot of stigma surrounding Ebola some families will not come forward when someone is sick for fear of being ostracised. This is also reflected in the fact that many of the local staff that I work with chose not to tell their families where they are working.
We seem to be getting lots of discharges, which is fantastic. It’s great to see survivors and we place a great emphasis on this. When they are able to clear Ebola and are strong enough for discharge, the patients will go to the “happy shower” to have their last chlorine wash, and leave all their personal belongings for incineration and collect new clothes. They are then able to leave the Red Zone for the outside world, where they are greeted by the local staff singing and dancing in celebration. They are given a discharge pack that includes money and food.
One particularly nice discharge was a brother and sister. There were lots of smiles, and they were fortunate to have a mother and father to take them home, which is not often the case. I see the discharge process as a very important part of letting the survivor know how special they are, and it helps in building community confidence. Not only that, but it does wonders for staff morale, as some of the things we see inside the gates are very unpleasant. It helps us remember the good work we are doing and the reason we are all here.