Yorkshire midwife says she would not be alive today if a family hadn’t agreed to donate their loved one’s liver to save her life


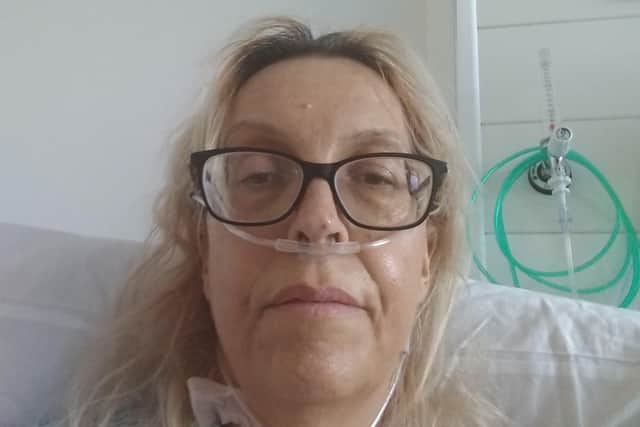
Midwife Ruth Clark says she has no words to thank the family of a woman who donated her a life-saving liver.
“Thank you just isn’t enough,” says Ruth, 50, from Thirsk. “All I know about my donor is that she was woman in her 30s. I have a daughter in her 20s and so I have so much empathy for them – they have lost a daughter, possibly a wife, mother and sister.
Advertisement
Hide AdAdvertisement
Hide Ad“But her family’s decision at such a time of grief to allow her organ to be used saved my life and means that my children still have a mother.”

It is a year since Max and Keira’s Law (Organ Donation (Deemed Consent) Act 2020) came into effect in England, which saw the country shift to an ‘opt out’ system for organ donation. The law means that people in England are considered as willing to donate, unless they have opted out, are in one of the excluded groups or have told their family they don’t want to donate.
“I really welcome the change in the law,” says Ruth, a mother of two. “But I do worry that families can still override the opt-out and refuse to let their loved one’s organs be donated. If the family of my donor hadn’t agreed to donate her organs I wouldn’t be here today.”
Ruth started to have health problems about 10 years ago.
“I started to suffer severe exhaustion,” she recalls. “I was going through a very stressful stage of my life; my marriage had broken down, I was bringing up two small children and retraining to be a midwife.”
Advertisement
Hide AdAdvertisement
Hide Ad

She went to her doctor for blood tests which revealed she was suffering from an autoimmune condition – PBC – primary biliary cirrhosis, which is a build-up of bile within the liver that damages the small bile ducts and causes cirrhosis
“They later changed the name to primary biliary cholangitis as people associate cirrhosis with alcoholism and this has nothing to do with alcohol.” As well as extreme exhaustion the condition can cause unbearable itching.
For a number of years Ruth was able to manage her condition which flared up at intervals and she was constantly monitored to check her liver function.
“I was working at St James’s Hospital in Leeds which was helpful as the hepatology department there is amazing.”
Advertisement
Hide AdAdvertisement
Hide Ad

But in 2018 colleagues started to mention that the whites of Ruth’s eye were starting to look yellow – a sign of liver failure.
“I had tried to ignore it but as I look for signs of jaundice in babies as part of my job I did realise that things weren’t right.”
Tests revealed that Ruth’s liver had deteriorated and the only treatment was a transplant.
Leeds is one of nine centres looking at using live donors who donate part of their liver and Ruth’s family were keen to be involved. But her liver was in such a bad way that she needed a full transplant and in January 2019 she was added to the national transplant list
Advertisement
Hide AdAdvertisement
Hide Ad“I was warned it could take some time. I am A negative – a rare blood group which only 14 per cent of the population has.”
In the end Ruth had her successful transplant on July 19, 2020, after two false alarms when she was in hospital but the livers were found not to be suitable.
“It is very hard waiting,” she says. “ You can’t go more than two hours away from the transplant centre which for me was Leeds, but by then I had also had to stop working which was hard as it is a realisation just how ill you are. It is also hard on your family.”
The pandemic made things worse as it meant Ruth also had to shield. But the six-hour operation was a success, and although she suffered some rejection and will need to stay on anti-rejection drugs for life, she is now looking forward to going back to work.
Advertisement
Hide AdAdvertisement
Hide AdBradford Teaching Hospitals’ organ donation committee chairperson, Karen Piotr, stressed how important it was for people to talk about their wishes before they die.
Her husband Mark died suddenly from a spontaneous and catastrophic brain bleed in 2017 aged 49. Through his death, Mark went on to donate his organs and help eight people.
Karen knew what Mark’s wishes were as they had talked about it many times before his sudden death and today she gets great fulfilment and satisfaction out of her work as a volunteer ambassador for NHS Blood and Transplant.
“Mark was my passion for over 30 years, so I wanted to talk about him and my experience of knowing his wishes so that others could be relieved of the burden of not knowing,” says Karen. “I wanted to encourage people to talk and share their organ donation decision, so becoming an ambassador was the opportunity to be able to do that.”
Advertisement
Hide AdAdvertisement
Hide AdMore recently nine-year-old Jordan Banks, who died after being struck by lightning, has helped three other children by organ donation.
In a message widely shared on Facebook, his father Matt described the young footballer as “the most amazing little person” with “the biggest heart” and said he had become an organ donor following his death.
He said: “Even now his kindness has meant that three other children may be able to live as he always told us he wanted to be able to help other people.”
Ruth has now written to her donor’s family and hopes one day she can meet them face to face to thank them for saving her life.
Advertisement
Hide AdAdvertisement
Hide AdMay 20 marks one year since Max and Keira’s Law (Organ Donation (Deemed Consent) Act 2020) came into effect in England, which saw the country shift to an ‘opt out’ system for organ donation.
Since the law changed 2,128,234 people in the Yorkshire region registered their organ donation decision on the NHS Organ Donor Register.
Of these, 1,943,408 has registered their support for donation, while 184,826 opted out
In terms of the population of Yorkshire, this means approx. 40 per cent have registered their organ donation decision.
Advertisement
Hide AdAdvertisement
Hide AdOf these, 36.6 per cent have opted in and 3.4 per cent have opted out.
www.organdonation.nhs.uk or call 0300 123 23 23
The next Transplant Games are being hosted in Leeds, in 2022 after being postponed this year due to the pandemic. Transplant Sport aims to raise awareness around the need for organ donation and to increase appreciation for donors and donor families.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.