Time to face up to ‘bizarre’ loopholes on cosmetic procedures
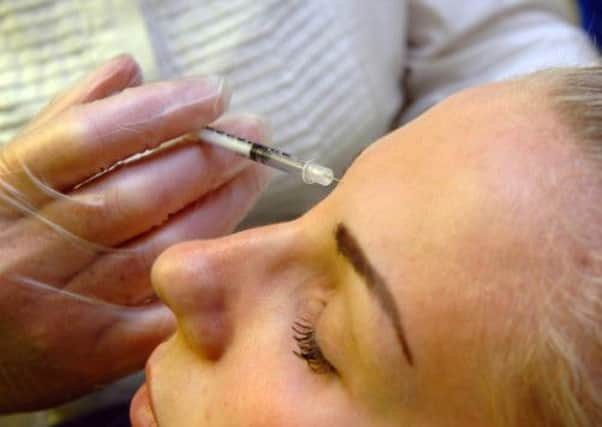

The market for cosmetic procedures is booming in the UK, with forecasts estimating that the £2.3bn spent in 2010 will rise to £3.6bn in the next two years.
An independent review has looked at the field and recommended a string of measures to protect patients better, particularly in the case of non-surgical procedures such as fillers to tackle wrinkles, Botox injections and laser hair removal, which the review described as “almost entirely unregulated”.
Advertisement
Hide AdAdvertisement
Hide AdCommissioned by the Department of Health in England, the findings will be passed to ministers across the UK and they are expected to form the basis of new legislation. They said these procedures could go badly wrong, were “trivialised” and treated as casually as having highlights done at lunchtime.
Sir Bruce Keogh, the NHS medical director for England who led the review said: “The most striking thing is that anybody, anywhere, any time can give a filler to anyone else and that is bizarre.”
Regulation to close legal loopholes is long overdue, says Professor Simon Kay, consultant plastic surgeon at Leeds Teaching Hospitals Trust. “The problem in this country is that cosmetic surgeons are split into reputable surgeons who are fixed in the landscape to a hospital and a community, and those who ‘fly in, fly out’ – offering no follow-up and proving difficult to find when something has gone wrong. Hopefully Brian Keogh’s review will help to tackle this.“
Prof Kay says a number of plastic surgeons have stopped using fillers because “the idea that they are harmless is completely wrong”.
Advertisement
Hide AdAdvertisement
Hide AdThey have their place, and the majority of the time their use is fine, but they can disfigure and ruin a life if done badly.
“There are good conventional alternatives (to fillers), such as rejuvenation surgery or injecting a person’s own fat.
“The filler industry has taken over because it is unregulated. The less responsible people who are using fillers and giving injections of Botox with very little training can disfigure a patient, yet they will have no indemnity insurance.“
The professor says the majority of practitioners who carry out procedures do it responsibly and well. The loopholes regarding regulation exist because no-one ever envisaged that anyone would carry out procedures on others without proper training, insurance and other safeguards. Patients should ask a lot of questions about qualifications, experience and insurance, and should be suspicious if a practitioner tries to rush them into any kind of discounted deal.
Advertisement
Hide AdAdvertisement
Hide AdDr Paul Charlson, who divides his time between general practice, dermatology and cosmetic practice in Hull, has fed his expertise into the Keogh Review. He says he hopes its string of recommendations – covering everything from making fillers only available on prescription to registration of everyone performing surgical and non-surgical procedures – will be incorporated into legislation. “It’s badly needed but we’ll see how workable the government considers the recommendations to be.”
Dr Charlson warns of some practitioners giving Botox that has been diluted so that its effects last a shorter time. “Usually if something is cheap there is a reason for it,” he says. “A website might claim ‘20 years’ experience’, but that might include only six months of cosmetic work.”