Why does no one want to talk about the F-word?

Most people just aren’t comfortable mentioning the F-word in public.
While around one in six UK couples have difficulty conceiving, the topic tends not to be discussed openly, which means it’s often a hidden struggle.
Advertisement
Hide AdAdvertisement
Hide AdSusan Seenan, chief executive of Infertility Network UK, says that around 3.5 million people in the UK have trouble conceiving.
“That’s a lot of people, and yet they’re not talking about it,” she adds. “We just want people to talk about infertility and understand that it’s not something to be ashamed of. It’s something you’re suffering from, and there’s help available.”
Seenan says many people lie about their reasons for not having children, because they feel embarrassed and a failure if they’re unable to conceive. And if there’s a medical problem with one partner, they will often feel they’ve let the other partner down.
“People shouldn’t blame themselves,” she says. “You wouldn’t be blaming yourself if you got pneumonia or another illness, but people feel their fertility is something they should be able to control and they can’t, so they feel ashamed, and want to keep this very personal issue to themselves.”
Advertisement
Hide AdAdvertisement
Hide AdInfertility can have many causes, including blocked fallopian tubes or endometriosis in a woman, a low sperm count in a man, or ‘unexplained infertility’, when tests find no obvious physical problems in the couple.
“Because there’s nothing apparently wrong, and nothing that can be treated, unexplained infertility can be even harder to deal with,” says Seenan. “And sometimes the more people worry, and the more focused they are on trying to conceive, the harder it can be to get pregnant.”
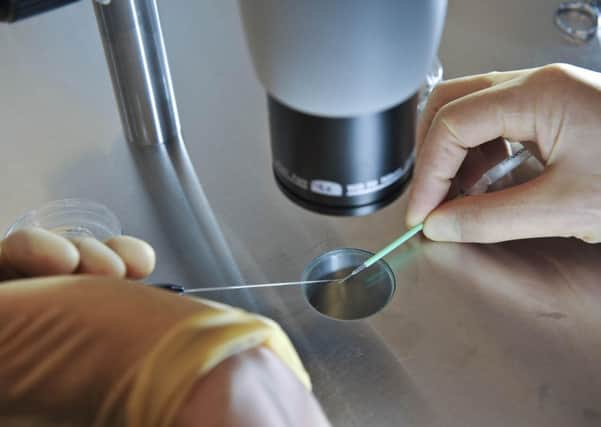
Various treatments are available, depending on the cause of infertility; for example, drugs may be taken to stimulate ovulation, or surgery may be needed to treat blocked fallopian tubes, endometriosis or male blockage problems. If these aren’t suitable or don’t work, many couples turn to IVF.
The number of IVF cycles performed each year has increased steadily since 1991, and the latest figures from 2011 show that around 47,000 women received treatment, with more than 60,000 rounds of IVF or ICSI being given; 4.3 per cent more than the previous year.
Advertisement
Hide AdAdvertisement
Hide AdIn 2010, the overall live birth rate per IVF/ICSI cycle was 24.5 per cent, which means that around three quarters of cycles don’t result in a baby - although clearly the more cycles a couple have, the better their chances of success.
NICE guidelines recommend offering three full IVF treatment cycles to women aged under 40 who’ve failed to get pregnant after two years of trying - although, largely due to costs, not every area offers this.
“Of all the people referred for IVF, some will be successful and a lot won’t, and many people aren’t prepared for that,” says Seenan. “You want people to be positive, but sometimes you have to be realistic as well. And there’s a postcode lottery for treatment, which is very cruel.”
Some couples feel they have no option but to pay for IVF privately. Costs vary, but can be anything from £5,000 per cycle upwards.
Advertisement
Hide AdAdvertisement
Hide AdThe process can be far more involved and draining - both physically and emotionally - than people realise, and can also put a strain on relationships.
“It’s important to stay relaxed, but also very, very hard to do that,” says Seenan. “The more you think about it, the harder it is. The impact fertility problems have is massively misunderstood. We want more support for people who are struggling to conceive, including better access to counselling. Sometimes people just need someone to talk to that understands.”
For more information about National Fertility Awareness Week, visit nfaw.org.uk or www.infertilitynetworkuk.com.