PTSD sufferer helped with new brain '˜rewiring' treatment

Gary Smith was just 17 when he started experiencing feelings of post traumatic stress disorder (PTSD), depression and anxiety.
Looking back he puts his low self-esteem and mental health problem to abuse first from a family friend when he was just a toddler and then later as a teenager by a man he worked for.
Advertisement
Hide AdAdvertisement
Hide AdTo cope with the PTSD symptoms in his late teens, Gary smoked marijuana and later started abusing ecstasy, amphetamines, cocaine and alcohol regularly on the weekends, to the point where he would often black out.


“I think I was a path of self-destruction for about four years, but also it helped to forget what had happened to me.”
As the years progressed, Gary, who has since moved to North Yorkshire, managed to kick his drug and alcohol habit. But his mental illnesses continued, and he would oscillate between feeling ‘normal’ and paranoid, with his sense of peace easily shaken by external circumstances.
During his lowest point, Gary was in the process of buying a house and experienced severe stress which triggered his PTSD.
Advertisement
Hide AdAdvertisement
Hide AdThis translated into him struggling to function at work – he would receive instructions from his manager which he’d forget the minute he walked away. In his personal life, he withdrew from family and friends, neglected his personal hygiene and states that he simply didn’t feel positive about life.
“It got the point where I just didn’t want to carry on. I couldn’t work, I didn’t want to go out and see anyone,” recalls Gary.
“Even though I had moved to an area where no one really knew me I felt that every time anyone looked at me they could tell what had happened to me all those years before and I felt ashamed. I carried it with me wherever I went. It changed the way I perceived other people and how I perceived myself.”
Eventually, with help from his partner of 18 years, Sarah, Gary sought help.
Advertisement
Hide AdAdvertisement
Hide Ad“When I looked into it, I realised that of the 16 symptoms of PTSD, I was suffering from 14 of them. I went to my GP for the first time and told her about how I perceived my symptoms and she agreed and started me on antidepressants – they did reduce my anxiety but did nothing to ease my depression. I could just cry for up to eight hours a day without being able to stop.”
After a year on the medication Sarah made enquiries with a family contact, Dr Leigh Neal, who recommended that Gary tried Transcranial Magnetic Stimulation (TMS) treatment.
“I’d been taking a number of different antidepressants but they really weren’t doing anything to help me at all. When my partner, Sarah, suggested I try TMS I was a point where I would try anything.”
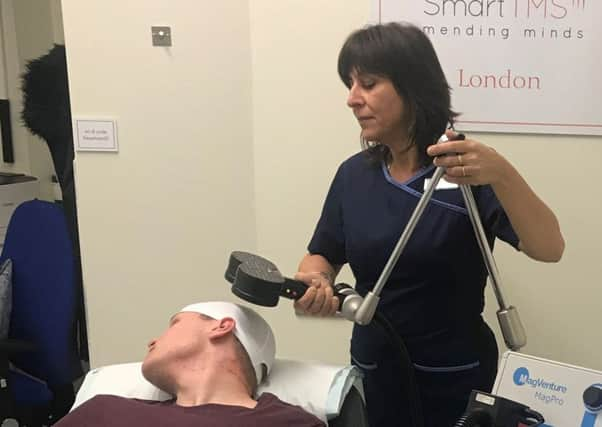
Repetitive transcranial magnetic stimulation (rTMS) involves placing an electromagnetic coil against a person’s head. The coil sends repetitive pulses of magnetic energy at a fixed frequency, which is delivered in pulses to specific areas of the brain. The stimulation can improve the symptoms of depression and anxiety. Scientists believe this encourages the area to “re-wire and grow more connections” in order to function properly again.
Advertisement
Hide AdAdvertisement
Hide Ad“I’d never heard of it, but it has been used in the US for 20 years, although it has only been approved in the UK for about two years,” says Gary.
“It is quite hard to described how the treatment feels, as it is done while you are awake with no anaesthetic, but it doesn’t hurt, it just feels like your head is being zapped.”
For Gary it was like a huge weight had been lifted off his shoulders.
After just three days of the treatment at the Smart TMS clinic in Manchester he started to feel the positive effects.
Advertisement
Hide AdAdvertisement
Hide Ad“I couldn’t believe it.I felt a smile returning to my face for the first time in years in place of the sadness I had experienced for so long. I started to feel human again.
And the feeling got incrementally better with the more sessions he had.
For the first time in 24 years, Gary now feels significantly better. He’s even started playing guitar and spending time outdoors again, and says his brain feels alive.
Gary had complex PTSD which is difficult to treat, according to Dr Neal, medical director and consultant in psychiatry and neuromodulation at Smart TMS.
Advertisement
Hide AdAdvertisement
Hide Ad“Gary suffers with a condition that is recognised by many psychiatrists as complex PTSD,” explains Dr Neal. “It is difficult to treat conventionally with psychological interventions and medication and many patients will remain chronically disabled by this condition for the majority of their lives.
“It is well established that rTMS is effective for depression and there is also now increasing evidence that it can help patients with PTSD.
“However, I was astonished to see the remarkable global recovery in Gary’s symptoms over the course of 30 sessions, such that he is now in full remission.
“This will require further research to properly establish its effectiveness in complex PTSD, but following my experience treating Gary, I would now have no hesitation in recommending rTMS to any patient with complex PTSD who has exhausted all the conventional recommended forms of psychiatric and psychological treatment. We now intend to keep Gary well with maintenance treatment once a month.”
Advertisement
Hide AdAdvertisement
Hide AdAs for Gary, he is hoping to be able to get back to work in the near future.
“This treatment has given me my life back,” he says.
Some names have been changed to protect the identities of those involved.
Repetitive transcranial magnetic stimulation (rTMS) involves placing an electromagnetic coil against a person’s head. The coil sends repetitive pulses of magnetic energy at a fixed frequency, which is delivered in pulses to specific areas of the brain.
When NICE looked at the evidence, it decided that transcranial magnetic stimulation for depression is safe enough and works well enough for use in the NHS.
Advertisement
Hide AdAdvertisement
Hide AdNICE looked at seven studies involving more than 6000 patients. Generally, the studies showed that the treatment improved depression symptoms and quality of life.
In some cases, it allowed patients to stop taking antidepressants altogether.