How the pandemic is redefining our NHS – Professor Mike Holmes

As a healthcare professional it has been the most difficult year of my career, but it is also a year that has taught me so much.
And whilst I certainly do not underestimate the challenges faced by our politicians, I’m sure there will be a time for political analysis in the future – my reflections are going to be much closer to home.
Advertisement
Hide AdAdvertisement
Hide AdOn an individual and family level we have felt a huge change to our lives. Freedoms that we would ordinarily have taken for granted have been restricted.


We have faced isolation – some more than others, we have been separated from our loved ones, we have had to work differently and many have been unable to work or lost their jobs.
We have faced suffering and bereavement on a scale that most have never experienced before. Schools have been closed, despite huge effort by our teachers, the education of our young people has been impacted.
It has genuinely been an annus horribilis by anyone’s standards. What it means to be both human and vulnerable has been brought sharply into focus.
Advertisement
Hide AdAdvertisement
Hide AdI have also witnessed huge change in the world of healthcare. In General Practice, we have seen a complete transformation of how we provide care – we have seen the population embrace technology and the introduction of remote consultations. There are pros and cons to this for sure.


However what I have seen is the way that my colleagues have strived to continue to deliver care with compassion despite the difficult circumstances. They recognise that human contact and human relationships are critical to do their job well.
There is a sad recognition that we may not be diagnosing, treating and referring all the illness in our community and that we are not able to optimise the wellness of that same community. Something that will need attention in the future.
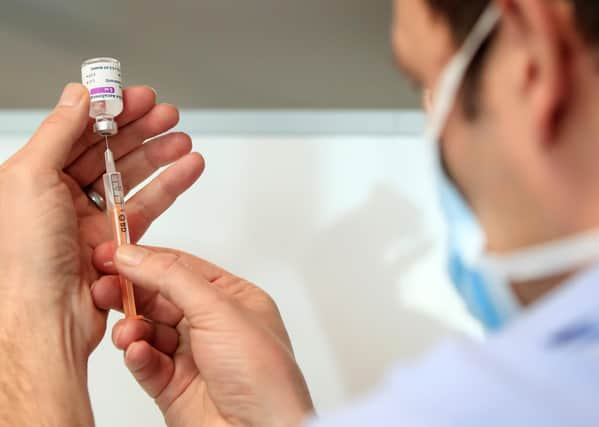
We’ve seen a phenomenal vaccination programme and the emergence of prioritising care according to risk as per the JCVI guidance – I suspect there are lessons to learn for us here as we emerge from the pandemic and try to get the NHS back to normal.
Advertisement
Hide AdAdvertisement
Hide AdOur hospitals have understandably played a central role in the last 12 months. As a GP, I look on this with enormous respect. Our colleagues in this sector have put themselves right in the path of the risk posed by coronavirus to help those who are suffering.
Their dedication and commitment have been inspirational, their compassion heart-warming. There has been no real let up throughout the year and they must be exhausted.
Nothing we can do, whether clapping or pay rises, can really be enough to acknowledge their contribution. They have been described as heroic – I’m not sure they are comfortable with that – in my view they are consummate professionals and genuine role models.
My hope is that they have inspired thousands of young people to choose healthcare as a career.
Advertisement
Hide AdAdvertisement
Hide AdOne thing I have observed during the pandemic is the level of collaboration that has been apparent particularly in the health and social care sectors. The willingness to support each other, the willingness to say yes.
My reflection is that this is, in part, due to the power of the single shared objective to get through the pandemic, stop people dying from Covid and return to something like normal.
There has been a desire to understand each other and a realisation that together we are stronger than the sum of our individual parts. I have seen first-hand with the vaccination centre in York just how this collaboration translates into reality and quality of care.
In summary, the last year has brought into focus that we are all human and vulnerable but that some in society can be more vulnerable than others. This disease has discriminated and has been more of a risk to the elderly, people from BAME communities and those living in deprived communities.
Advertisement
Hide AdAdvertisement
Hide AdWe have seen that we can adapt, that we can change our behaviour and that we are resilient – no matter how difficult has been.
My sense is this will change our lives forever but that we will come out of it having learned so much.
Professor Mike Holmes is a GP Partner at the Haxby Group and Chair of Nimbuscare.
Support The Yorkshire Post and become a subscriber today. Your subscription will help us to continue to bring quality news to the people of Yorkshire. In return, you’ll see fewer ads on site, get free access to our app and receive exclusive members-only offers. Click here to subscribe.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.