'Far greater' investment needed in rural GPs, Yorkshire peer warns
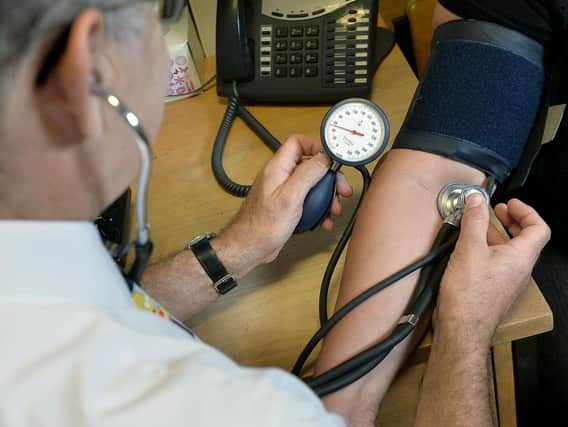

A Yorkshire peer has claimed that GP surgeries in rural locations such as along the region’s coastal areas are facing funding issues which are causing additional challenges on hospitals.
Baroness Anne McIntosh of Pickering, who sits in the Lords for the Conservatives and who had GPs in her family, told The Yorkshire Post “there needs to be far greater investment in rural GPs” to prevent people ending up in hospital when they could have been treated locally.
Advertisement
Hide AdAdvertisement
Hide AdShe explained: “There used to be a formula used which recognised the rurality and sparsity factors in rural areas which attracted additional funding, recognising the long distances between patients and their doctors, as well as bad weather in winter in many rural areas, meaning GPs are not so accessible.
“That is no longer recognised in the funding with the perverse effect that patients are being taken into hospital as an emergency in a way that could be entirely preventable. The funding needs to be distributed more fairly between primary and secondary care to ensure that the quality of health care is equal as well as between urban and rural areas.”
Her warnings come just weeks after England’s Chief Medical Officer Professor Chris Whitty called for a national strategy to improve healthcare in coastal communities, and said that “communities have often been overlooked by governments and their ill-health hidden because their outcomes are merged with wealthier inland areas”.
The report detailed how coastal communities are looked after by fewer NHS staff than the national average, with recognition that “the training of doctors at both undergraduate and postgraduate levels has not always aligned with healthcare need, contributing to health inequalities”.
Advertisement
Hide AdAdvertisement
Hide AdData from the BMA (British Medical Association) shows that the number of fully qualified GPs working the equivalent of full time hours has fallen nationally by more than 1,300 between 2015 and early 2021.
The number of senior GP partners - generally older and more experienced - is also falling, with a reduction of 546 doctors between March 2020 and March 2021.
Shadow health minister Justin Madders said the pandemic has “shone a light” on the health inequalities that have long-existed across the country.
He said: “The Government’s planned top down reorganisation of the NHS could have solved these challenges - but instead there was no plan to tackle these stark inequalities, no plan to recruit and train more doctors and nurses and no plan to bring down waiting lists.
Advertisement
Hide AdAdvertisement
Hide Ad“Far from levelling up, the Tories are neglecting the health of rural communities, and their plans for NHS reform will only make this worse. “
Health Secretary Sajid Javid has previously said he will “carefully consider” Professor Whitty’s recommendations in his report.
At the time of its release he commented: “Those living in coastal areas clearly face different sets of challenges to those inland but everybody, no matter where they live, should have similar opportunities in education, housing, employment and health.
“We are committed to levelling up across the nation and the new Office for Health Promotion – launching in the autumn – will drive and support the whole of government to go further in improving people’s health.”