Exhausted doctors need support over NHS recovery – Dr Chaand Nagpaul
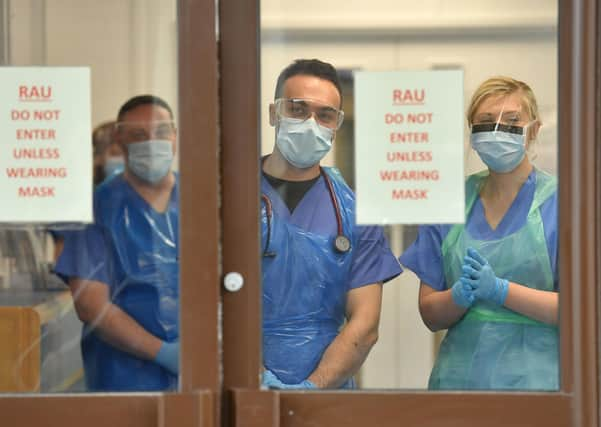

So while the Government highlights the scale of the backlog and need to restore services, the £1bn funding already committed is nowhere near what is required, with the BMA estimating that it will cost at least £4bn to clear the elective backlog alone.
Meanwhile, sweeping upheaval to the health service at this time mustn’t be allowed to distract from this urgent task at hand.
Advertisement
Hide AdAdvertisement
Hide AdThe BMA has long supported greater collaboration within the NHS but we must continue to question the timing of the Government’s legislation as doctors and their colleagues need ample opportunity to engage with these changes.


Clinicians, who know their communities and where barriers to greater integration lie, must be given the chance to locally lead changes that benefit both staff and patients.
It is these same staff who will be instrumental in tackling the record-high waiting lists.
But we came into the pandemic with an historic workforce crisis, with significantly fewer than our European counterparts, and now a growing number of our members tell us they’re planning on leaving the NHS due to the distressing and exhausting experiences of the last year.
Advertisement
Hide AdAdvertisement
Hide AdWhile earlier commitments made in the White Paper say the legislation will place a duty on the Secretary of State to take more responsibility for workforce planning, this must be backed by the Government guaranteeing that staffing levels safely meet the needs of the population – and providing whatever funding and resourcing this requires.


The NHS has for too long been beleaguered by bureaucracy that has obstructed care. It makes no sense that our National Health Service has to put all contracts out to competitive tender – something the BMA has campaigned against since 2012.
The Government is taking the first step towards abolishing these wasteful rules, but unless it goes further – making the NHS the default option for delivering NHS services – there is a risk that contracts will be awarded without scrutiny to private providers at huge expense to the taxpayer, as was seen with the procurement of PPE and Test and Trace during the pandemic.
It’s vital that the Government sticks to its pledge to address the longstanding and urgent crisis in social care by the end of the year. Without doing so threatens both the health and wellbeing of thousands of vulnerable people and continued knock-on effects on the health service.
Advertisement
Hide AdAdvertisement
Hide AdDoctors know that prevention is better than cure, and commitments to tackling areas of poor health that have been so visibly exposed during the pandemic – including obesity – are positive.
However, with public health services undergoing years of savage cuts, these will only be achievable with substantial investment in public health infrastructure and staffing, which the BMA has long called for.
After the year that healthcare workers have endured, witnessing loss of life on a scale previously unimaginable, we need decision-makers to be held accountable.
It’s right then that accountability for the NHS is placed firmly at the door of Government in this legislation. However, protection must be put in place to prevent this being used to secure more power over the health service for political ends.
Advertisement
Hide AdAdvertisement
Hide AdSince its inception, the NHS has been subject to countless reorganisations, only for these to be abandoned or replaced as soon as those in power choose to do so.
This is an opportunity to improve our health service and the health of the nation, but it must be solely driven by a desire to help patients, and to ensure that the NHS is given long overdue investment and support to be a publicly-funded provider to care for the health needs of our population.
Dr Chaand Nagpaul is the British Medical Association’s council chair.
Support The Yorkshire Post and become a subscriber today. Your subscription will help us to continue to bring quality news to the people of Yorkshire. In return, you’ll see fewer ads on site, get free access to our app and receive exclusive members-only offers. Click here to subscribe.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.