Listen to GPs over appointments, Sajid Javid – Jayne Dowle
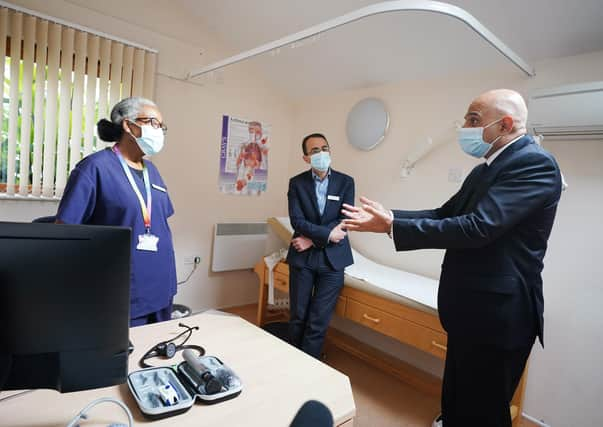

He’s also putting more onus on advanced nurse practitioners, physiotherapists and community pharmacists to diagnose problems and divert care.
Advertisement
Hide AdAdvertisement
Hide AdOn paper, it sounds positive, but hold on a minute. How has the NHS ended up with a black hole of £250m in its funding in the first place? I’d be very interested to know how the money will be apportioned to pay for it.


The pandemic, you say? Well of course. Our health services have been under unprecedented pressure for almost two years now. We all know that.
However, we also know that the Department of Health and Social Care exists for a reason; presumably, amongst its responsibilities, it should ensure that the services it provides are predicted, analysed, costed and carefully decided upon. Didn’t anyone see this £250m shortfall coming?
Advertisement
Hide AdAdvertisement
Hide AdOr were Ministers and mandarins so preoccupied with the £37bn cost of the Test and Trace system, set up in May 2020, that the day-to-day work of NHS family doctors rapidly became sidelined?


That Test and Trace has been judged as a failure adds insult to injury, especially as its premise, to avoid a second national lockdown, clearly failed. Two further lockdowns followed and had an impact on the recovery of the economy by taking people out of the workforce.
If this winter access fund announcement was intended as a grand gesture to appease a weary and frustrated public and restless and exhausted GPs, it has clearly backfired.
Leeds doctor Richard Vautrey, the chair of the BMA’s GPs committee, slams the Government’s preoccupation with face-to-face appointments as a populist move which fails to recognise the scale of problems on the ground.
Advertisement
Hide AdAdvertisement
Hide Ad“It is… disappointing to see that there is no end in sight to the preoccupation with face-to-face appointments,” he said before calling for “a more intelligent conversation about the variety of appointments and care that are available to patients to meet their needs”.
And rightly so. Whilst older and vulnerable patients, and parents of young children, do appreciate being able to see their doctor in person, and should be given precedence, many of us do recognise that virtual appointments for less urgent issues can be effective.
Our shared priorities, surely, should be for GPs to be available to help their patients, in whatever way.
I’ll tell you a story about priorities. Last week, my husband was called into the health centre for a blood test.
Advertisement
Hide AdAdvertisement
Hide AdHe suffers from rheumatoid arthritis and hasn’t seen either his GP or hospital consultant for months, with repeat online prescriptions the only contact.
He naturally assumed that this blood test would be to measure levels for RA, presumably so he could be eventually seen either in surgery or at a hospital clinic.
He took an hour and a half off work and phoned me afterwards, perplexed. Turned out that his trip to the doctors had nothing to do with his clearly diagnosed degenerative condition; rather, as he recently turned 50, it was to take blood to check whether he might be at risk for diabetes.
Diabetes? Yes, I know it is a dangerous condition and that a few lifestyle changes can halt its onset. Really though? Is that kind of appointment a priority, when so many cases of cancer diagnosis are being missed because people can’t get to see a doctor and waiting lists for treatment stretch into years?
Advertisement
Hide AdAdvertisement
Hide AdSomeone sanctioned him spending almost half an hour with a nurse practitioner – for what?
And let’s not forget, as of last week, 277,875 people in the UK had tested positive for coronavirus, an increase of 13 per cent in a week. Possible risk of diabetes vs tackling a pandemic. Which one would you choose?
Mr Javid might like to heed this as an example of the frustrations felt by both the public and GPs. Both the British Medical Association and Royal College of GPs suggested suspending the Quality Outcomes Framework, under which GPs are paid for monitoring patients who suffer from, or are at risk of, conditions such as diabetes and asthma.
Other ideas they proposed to reduce workloads included creating a new national helpline to answer queries about Covid vaccination, and for hospitals to set up systems to let patients know when their planned surgery is happening, to reduce chasing calls to GPs.
Advertisement
Hide AdAdvertisement
Hide AdAll this, however, would demand a high level of engagement and communication between the Health Secretary and multiple agencies of the NHS. Far simpler to throw money at the problem and hope it will go away. I have news for Mr Javid. It won’t.
Support The Yorkshire Post and become a subscriber today. Your subscription will help us to continue to bring quality news to the people of Yorkshire. In return, you’ll see fewer ads on site, get free access to our app, receive exclusive members-only offers and access to all premium content and columns. Click here to subscribe.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.